Diagnosis & Treatment
Eczema in skin of color can look different than on white skin. The diagnosis is often more challenging. Symptoms on dark skin are sometimes overlooked.
Familiarity with how eczema looks in skin of color is essential in making a correct diagnosis and prescribing the right treatment.
Allergists and dermatologists are specialists trained to diagnose and treat skin conditions, including eczema, also called atopic dermatitis (AD). AD is a form of eczema that is related to allergies that cause skin symptoms.
Diagnosing Eczema on Darker Skin Tones
Many images of eczema you see online or in publications often show redness, red dots or red bumps on lighter skin tones. The presentation of eczema on darker skin tones is different from the classic “red rash” often shown in photos.



What does eczema in skin of color look like?
In people with black or brown skin, eczema may appear as dark brown, purple or ashen gray rashes or patches. Sometimes, it can appear as small bumps or dry skin. These symptoms may be harder to recognize.
Because of these differences, people with darker skin may wait longer to get the right diagnosis. If doctors are not used to seeing eczema on darker skin, they might mistake it for other conditions like psoriasis or fungal infections.
Common eczema symptoms across all skin colors
These common signs are universal across different skin tones and can help doctors confirm an eczema diagnosis:
- Itchy rash (often intense)
- Swelling or inflammation of affected skin
- Dry skin
- Cracked or scaly patches of skin
- Skin that feels warm when touched
- Open, oozing, weeping, or crusty sores
Eczema in brown or black skin
On darker skin types, eczema can have additional or different signs:
- Color changes: Skin patches may appear brown, purplish, gray, or ashen instead of red.
- Follicular accentuation: The skin around hair follicles becomes bumpy and resembles goosebumps. This can cause thickened or firm skin, with hair standing on end.
- Papules: Small, raised bumps, often found on the arms, legs, chest or back.
- Lichenification: This occurs with frequent scratching, causing skin thickening and toughness. In some cases, raised bumps called prurigo nodules can develop in these scratched areas.
- Skin discoloration (pigment changes): After a flare-up, the skin may darken (hyperpigmentation) or lighten (hypopigmentation). These changes can be very noticeable on darker skin tones. They can often cause distress or anxiety, especially for teens. Regular treatment can help return skin pigmentation to its usual color, but it can take months or years to fully fade away.
It’s common for eczema symptoms in people of color to be misdiagnosed as another condition. A misdiagnosis or delayed diagnosis can lead to no treatment or the wrong treatment. It can also increase the risk of hypopigmentation as the surrounding skin heals after an eczema flare.
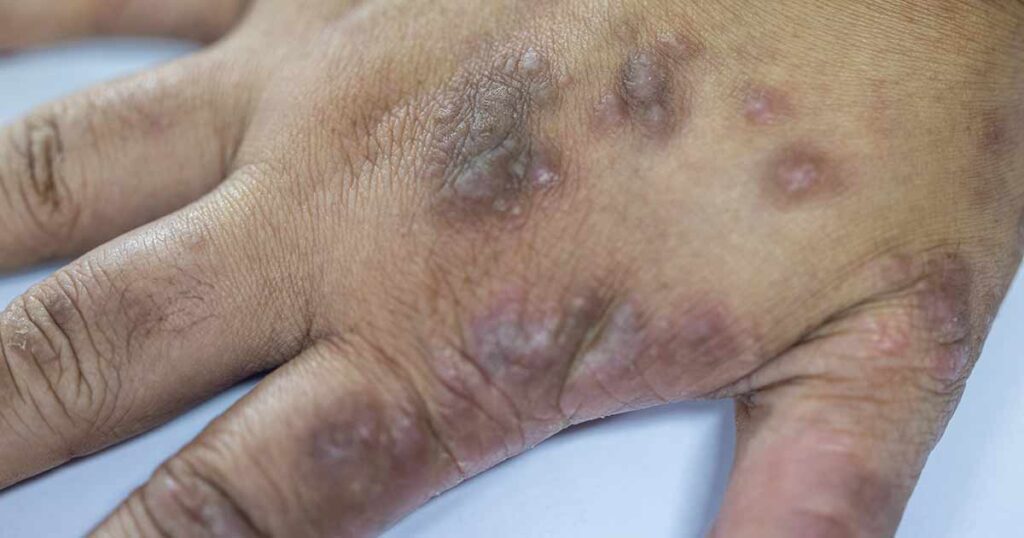
Diagnosing Eczema in Skin of Color
Your doctor will examine your skin for symptoms of eczema. For people with skin of color, the doctor will pay special attention to any skin color changes and bumpy or thickened areas.
The doctor will also take your detailed medical history and ask about:
- Family history of eczema, allergies, or asthma.
- Lifestyle factors such as stress levels or the environment you live in.
- What makes your eczema worse — are you using products known to cause eczema flares, for example.
Common triggers include:
- Allergens: pollen, mold, foods, dust mites, dog or cat dander
- Personal hygiene products: shampoo, cosmetics, beauty products, hair products
- Harsh chemicals: soaps, detergents
- Irritants: wool, nickel
- Environmental factors: dry climate, exposure to extreme cold or hot temperatures
- Lifestyle: stress, change in environment, work environment
Testing Used to Diagnose Atopic Dermatitis
As part of a diagnosis, your doctor may perform tests to identify if there’s an allergen or irritant causing symptoms.
Skin prick test. In a skin prick test, a doctor or nurse gently pricks your skin, usually on your back or forearm. A small amount of a diluted allergen is then placed on that spot. After 15 minutes, the doctor checks for a bump (wheal) or color change (flare). A reaction shows there is a sensitivity to that allergen. Several allergens can be tested at once.
Note: In most cases, you must stop taking antihistamines for at least 3 days before this test. The test is commonly done on your first visit to a doctor.
Blood test. A small sample of blood is taken and checked for IgE antibodies specific to an allergen. IgE levels will be high if your body reacts to certain allergens. Some tests may measure a specific allergen, or overall levels of IgE. Sometimes, a doctor orders a more detailed test that checks the specific components of an allergen. Lab results usually take a few days to come back.
Patch test. For a patch test, adhesive strips with small chambers of chemicals are placed on your back. After 2–3 days, the patches are removed, and the skin is checked. If symptoms appear, then it’s confirmation of an allergy. Patch testing is commonly used for contact allergies to fragrances, detergents, metals and other chemical sensitizers.
Oral food challenge. If your doctor thinks certain foods are causing eczema to flare, you may be asked to take an oral food challenge. In an oral food challenge, you eat a tiny amount of a suspected allergen. Then you gradually eat more as the doctor monitors you for allergic reactions. An oral food challenge should only be conducted by a doctor. It should only be done at a medical facility that has access to emergency epinephrine in case of a severe allergic reaction.
Special considerations for allergy testing in children with eczema
Children under five years old who have moderate to severe eczema may need extra testing, especially if their symptoms do not improve with initial treatment. They may be tested for food allergies to:
- milk
- egg
- peanut
- tree nuts
- wheat
- soy
- sesame
- fish
- shellfish
Babies with severe eczema are at high risk for developing severe food allergies (particularly peanut) in early childhood. These infants should see a pediatrician, allergist or dermatologist. Guidelines say they can start eating peanut-containing foods starting at 4-6 months of age to help prevent peanut allergy.
It is important to know that eczema, while chronic, can come and go.
NOTE: About one-third of young children with moderate to severe atopic dermatitis may have a food allergy.
Other tests that may be used to rule out an eczema diagnosis
- Filaggrin exams and buccal swabs: these are used to detect mutations in the filaggrin gene, the protein that helps protect the body from allergens and bacteria. A lack of filaggrin weakens the skin barrier, leading to eczema.
- Skin biopsy: this is used to rule out other skin diseases, including psoriasis or cancer. In a biopsy, a tiny piece of skin is removed and analyzed under a microscope.
Eczema Treatments
Eczema treatment is the same for all patients, regardless of skin color. There is no cure, but there are medications to help relieve symptoms and reduce flare-ups.
Since misdiagnosis of eczema can occur in people of color, treatment may begin later with symptoms that are more severe. Symptoms may also be more persistent as a result.
An allergist can work with you to develop an eczema treatment plan. The goal is to enable patients to lead a comfortable, normal life with fewer or no symptoms.
Treating eczema often begins with moisturizers and gentle skincare. If symptoms are still moderate or severe, your doctor may prescribe stronger creams or ointments. These may include topical corticosteroids.
When even more control is needed, medications that work on the whole body (systemic), like biologics or oral JAK inhibitors, are considered.
Work with your doctor to develop a personalized treatment plan. It can be based on your skin type, lifestyle, and any other risk factors.



Moisturizers and basic eczema care
Eczema treatment starts with over-the-counter or prescription topical skin moisturizers. Medications include over-the-counter or prescription anti-inflammatory creams and ointments. These help protect the outer layer of the skin by sealing in moisture and combating dryness. They keep out allergens, irritants and bacteria and prevent flare-ups. They help soothe the skin for long-lasting hydration.
Doctors recommend applying a moisturizer at least twice a day, including once after a bath or shower. Patients and caregivers can develop a schedule so that moisturizing becomes part of a daily skincare routine.
Mild cases of eczema can be treated with petroleum jelly. These should be applied daily, even when the skin appears clear, to help prevent dryness.
Soak and seal
For children with severe eczema, allergists advise using the “soak and seal” treatment. Soak and seal can provide relief from the itching that comes with eczema. Here’s how it works:
- Bathe in lukewarm water at least once a day. (Doctors recommend short baths for eczema.)
- Use an unscented, dye- and fragrance-free cleaner. No soap.
- After bathing, gently pat the skin dry.
- Immediately apply moisturizer to “seal” in moisture.

Topical treatment for eczema on skin of color
In cases of moderate or severe disease, an allergist may prescribe a topical cream or ointment. These medications help reduce skin inflammation, relieve itch, combat dryness, and prevent flares from reoccurring.
Topical corticosteroids
- Helps reduce inflammation and itch, and prevent flare-ups.
- Many topical corticosteroids are available, ranging from mild to very strong.
- Your doctor may recommend other topical options for long-term use.
Topical calcineurin inhibitors
- Suppresses the protein calcineurin that causes skin inflammation, reducing itching and inflamed skin.
- Approved for adults and children ages 2 and older.
- Less risk of skin thinning compared to topical corticosteroids.
- Often used on sensitive areas (face, neck, skin folds).
- Examples: Tacrolimus (Protopic®), Pimecrolimus (Elidel®)
PDE4 inhibitors
- Targets PDE4 enzymes which cause inflammation deep within the skin, it works by reducing swelling and inflamed skin.
- Well-tolerated for long-term use.
- Approved for mild to moderate atopic dermatitis.
- Examples: Crisaborole (Eucrisa®), Roflumilast (Zoryve®)
- Crisaborole is for adults and children 3 months of age and older. Rofulimilast is for adults and children 6 years of age and older.
Topical aryl hydrocarbon receptor agonist (Tapinarof)
- Attaches to a special receptor in the skin called the aryl hydrocarbon receptor (AHR).
- Helps reduce inflammation and cell damage, and build up proteins that keep the skin barrier strong.
- Approved for adults and children 2 years of age and older with eczema (atopic dermatitis).
- Brand Name: Vtama®
Topical Janus Kinase (JAK) inhibitors (creams)
- Blocks enzymes involved in the immune response. These medications reduce inflammation, itchy skin, and scaly skin.
- JAK inhibitors alter the immune system’s ability to react to germs. As a result, some people on these medications may be at risk for bacterial, fungal or viral infections. Talk with your doctor about the benefits vs. risks of taking JAK inhibitors.
- Examples: Ruxolitinib (Opzelura®), Delgocitinib (Anzupgo®). Both are applied to the skin as creams.
- Opzelura is approved for moderate to severe eczema in adults and children 12 years of age and older who have not responded well to other topical medications. Opzelura is also approved for mild to moderate eczema in children ages 2 to 11. Anzupgo is approved to treat chronic hand eczema in adults.

Biologic medications for severe atopic dermatitis
If eczema is still difficult to control after topical treatments, the next step may be an FDA-approved biologic medication. This is for patients whose symptoms are not well-controlled by topical therapies. Biologics can be used in combination with topical corticosteroids and/or calcineurin inhibitors.
- Dupilumab (Dupixent®), approved for 6 months and older
- Tralokinumab (Adbry®), 12 years and older
- Lebrikizumab (Ebglyss™), 12 years and older, weighing over 40 pounds
- Nemolizumab-ilto (Nemluvio®), 12 years and older
Oral medications to treat eczema (pills or tablets)
Short courses of oral corticosteroids
- Used to quickly control severe eczema flares. (Some people may experience a worsening of symptoms again after treatment ends.)
- Not for long-term use because of side effects (e.g., weight gain, high blood pressure).
JAK inhibitors (oral pills)
- Blocks enzymes involved in immune response.
- For moderate to severe eczema in people 12 years and older who have not been helped by other treatments.
- JAK inhibitors can raise the risk of infection, so talk about benefits vs. risks with your doctor.
- Examples: Abrocitinib (Cibinqo®), Upadacitinib (Rinvoq®)
Antihistamines
- Relieves itching and helps with sleep — especially beneficial for children who scratch at night.
- Do not treat the cause of eczema. They help manage symptoms.
Other atopic dermatitis therapies
Wet wrap therapy
- Used to help eczema by hydrating the skin, relieving itching, and allowing healing.
- How it works: After a soak-and-seal bath and applying topical moisturizers or creams, wrap the affected skin in a wet cloth. Then cover it with dry clothes (pajamas, sweatshirts or tube socks).
Bleach baths (or vinegar baths)
- A bleach bath can help kill bacteria and prevent infection if properly diluted and used as directed.
- Most effective when combined with moisturizers and medications.
- How it works: Add a half-cup of regular household bleach (not concentrated) or a cup of vinegar to a full tub of water. Soak for 10 minutes and then rinse off before applying moisturizer. Keep the bleach out of reach of children.)
Light therapy (also called phototherapy)
- Light therapy is an in-office procedure that involves exposing eczema-damaged skin to ultraviolet (UV) light.
- Reduces inflammation and itch, and boosts the body’s bacteria-fighting ability in hard-to-control eczema.
- Important note: light therapy can cause hyperpigmentation (darkening of the skin) in people with darker skin. It’s important for doctors and patients to fully discuss the benefits and side effects of this treatment.

Tried-and-True Atopic Eczema Management Tips
Daily skincare routines to manage eczema
- Moisturize often. Use at least twice a day, especially right after bathing, to lock in moisture.
- Take warm baths, not hot. Adding fragrance-free bath oil, salt, baking soda, or uncooked oatmeal can ease severe itching.
- Use soap-free cleansers. Gentle, detergent-free products are less likely to dry out the skin.
Clothing and fabrics
- Avoid irritating fabrics. Stay away from wool or rough materials that worsen itching.
- Choose loose-fitting clothes. Tight garments can rub or irritate the skin, causing a flare or not allowing the skin to heal.
- Protect your skin from cold weather. Wear gloves to keep skin from dryness and cracking.
Avoiding scratching
- Cover itchy areas. Helps prevent picking or scratching, allowing the skin to heal.
- Avoid scratching directly. If you must touch an itch, press lightly or use the back of your hand instead of nails.
- Keep nails short. This can minimize the skin damage if they try to scratch.
Lifestyle and environment
- Identify and avoid triggers. If you know certain things trigger severe flare-ups, make necessary changes to avoid them.
- Stay hydrated. Drink plenty of water to help your skin hydrate from the inside out.
- Run a humidifier. Add moisture to indoor air, helping to prevent dryness.
- Mind the environment. Keep your living space from getting too dry or too hot.
- Manage stress. Stress can trigger flares; try counseling, relaxation techniques, or support groups.
Additional resources

Eczema Medications and Treatment Options– Allergy & Asthma Network

Coping with Eczema– Allergy & Asthma Network